Deep Anterior Lamellar Keratoplasty for
The patient is a 22 year old male that presented as an outpatient to our clinic with complaints of low visual acuity of his left eye.
He had a history of recurrent episodes of epithelial keratitis on is left eye, attributed to Herpes simplex virus (HSV) infection. He had undergone several treatment courses with both oral acyclovir and topical acyclovir ointment.
Despite reporting a remarkable improvement of his complaints of pain, weeping and burning sensation, he noted a marked decrease of vision.
At the time of the visit he was still being treated with prophylatic oral acyclovir.
The patient has a long-standing history of atopy with some bouts of seasonal allergic conjunctivitis.
He also suffers from Keratoconus. Assessment of his right eye showed progression to stage 3 in the Amsler-Krumeich classification. He had progressively become intolerant to contact-lens use and presently uses spectacle correction.
On physical examination, our patient's best corrected visual acuities was 3/10 in the right eye, using a spectacle correction of 12,5(-5,5 x 40)
Visual acuity of his left eye was limited to hand motion perception.
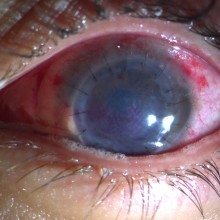
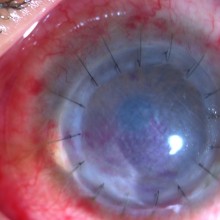
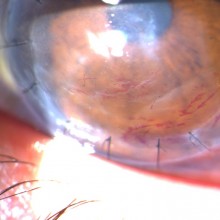
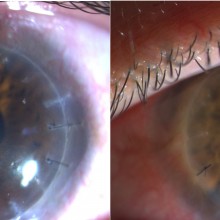
Slit lamp examination of the left eye showed conjunctival injection and a diffuse decrease of corneal transparency, central lipid keratopathy and deep stromal neovascularization of the inferior third of the cornea.
Anti-viral prophylaxis was continued.
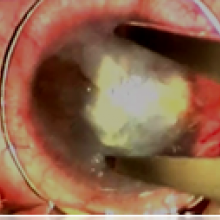
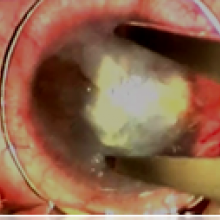
After careful consideration, it was decided to perform a deep anterior lamellar keratoplasty (DALK) on the left eye of the patient, aiming at restoring corneal transparency.
Although a full-thickness penetrant keratoplasty is commonly performed for the treatment of deep corneal scars, in some cases of corneal scarring due to HSV keratitis, DALK has proven to be a valid alternative. (1)
Since the corneal endothelium appeared healthy, the option for DALK instead of PK was based on the prospect of:
1- faster visual rehabilitation
2- lesser post-keratoplasty astigmatism
3- sustained mechanical integrity of the anterior surface
4- lower endothelial rejection risk
On the first day after surgery, the patient's visual acuity had improved to 2/10 with no correction.
Slit lamp examination revealed some small traces of blood on the graft-host interface, stromal edema, and a small central corneal ulcer.
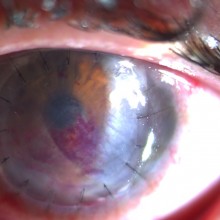
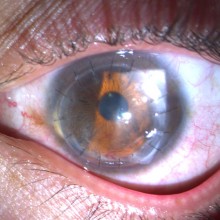
On the sixth post-operative week, best corrected visual acuity had improved to 6/10 using +0,75 (-4,75 x 180º). Slit lamp examination showed only vestigial amounts of blood on the interface and a small inferior scar.
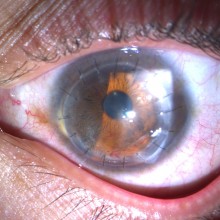
After 5 months, the patient presents a best corrected visual acuity of 8/10 using -0,5 (-3,5 x 15º)
The graft is fully transparent, with no trace of hematic staining.
In this particular case, the option to perform DALK proved to be a safe and efficient alternative for the rehabilitation of post-herpetic corneal scarring.
Visual recovery has been remarkable and there were no episodes of infectious recurrence or graft rejection during the observed follow-up.
1- Sarnicola, V. et al : Deep anterior lamellar keratoplasty in herpes simplex corneal opacities. Cornea 2012